Essential Diagnostics
The TMD doctor must have all the essential diagnostics at his disposal in order to facilitate “differential diagnosis”. Relying on yesterday’s diagnostic protocols inevitably results in yesterday’s treatment results, which were notoriously ineffective. Poor treatment, ineffective treatment, and mis-treatment is the result of many TMD doctors just repeating their mistakes.
This multi-dimensional means of observing typical signature patterns confirming injury incorporates several of our senses, exponentially enhancing our spatial visualization and conceptual grasp of the functioning or dysfunctioning of body parts, organs, and neurovascular systems, while utilizing to the fullest the physical findings from the clinical examination of the patient.
- Functional JVA accurately measures and locates TMJoint sounds in function.
- Functional EMG accurately measures the activity in muscles in microvolts.
- Functional EGN accurately measures the motion and range of movement of the mandible in function.
NO ONE TEST CAN CONFIRM THE DIAGNOSIS OF TMD; BUT WHEN INTEGRATED TOGETHER WITH THE CLINICAL EXAM AND RADIOGRAPHS, IT CAN CONFIRM AND RE-CONFIRM THE DIAGNOSIS.
Functional Joint Vibrational Analysis (JVA)
When a patient is suffering from TMD (temporomandibular joint dysfunction), there are often noises emanating from the temporomandibular joints which indicate on-going tissue damage of the temporomandibular joint mechanism.
Joint Vibration Analysis (JVA), sonography, sonar, auscultation (stethoscope), and palpation are the usual ways of auditing these noises. However, JVA is the most accurate means of measuring these interferences in TMJoint function as it is the only method which allows the clinician to differentiate between sounds in the left joint, the right joint or whether there is independent sound or noise in both TMJoints. In addition, these major interferences can be accurately measured determining which tissues are being damaged. Henceforth we will refer to these TMJoint noises as MMI (Major Measured Interferences during TMJoint function).
Hawaii TMJ Institute utilizes JVA from a Bio-Research Sono-Pak measuring intracapsular TMJoint sounds (major measured interference) against normalized data, duration of these sounds, and exact location of the occurrence of these sounds during jaw opening/closing, or lateral excursions, and a spectral frequency analysis of the sound using FFT. Without this information, one could not restore function free of intra-capsular interference.This objective functional testing readily differentiates normal temporomandibular joint function from compromised temporomandibular joint function.
Functional Electromyograhpy (EMG)
As a result of pain elicited in palpating muscles and areas of the craniomandibular complex, and in consideration of the patient’s complaints, an Electromyography (EMG) series to more specifically delineate and define hypertonic musculature is recommended. This series was necessary in order to differentially diagnose between intra-capsular interference (meniscal or otherwise) and extra-capsular interference (influence of the surrounding hypertonic muscular matrix) so as to determine the predominant dysfunctions. Defining the etiology of this patient’s predominant neuromuscular dysfunctions can help preclude misdirected palliative treatment regimens.
Electromyography (EMG) utilizes eight channels monitoring the right and left sternocleidomastoid muscles, right and left anterior temporalis muscles, right and left masseters, and right and left anterior digastric muscles.
Functional Electrognathography (EGN)
Electrognathography (EGN) measures vertical dimension, extent of lateral deviation upon opening and position where the deviation occurred, mandibular opening and closing movement pattern during function from a frontal and sagittal view, velocity of jaw motion at incisal reference point during jaw opening and closing movements, and evenness or smoothness of jaw movements as opposed to jerking or uneven motion. This series is necessary to determine how the extra-capsular interference of the surrounding hypertonic muscular matrix contributes to dysfunction.
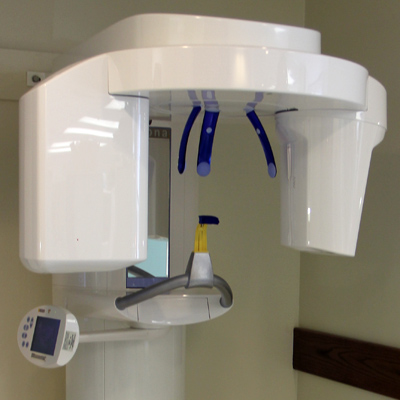
Cone Beam Computed Tomography (CBCT)
Cone Beam Computed Tomography (CBCT) has proven to be one of the most reliable imagery in the diagnosis of patients suffering from Temporomandibular Dysfunction and Craniofacial pain. Tomography provides clinicians with layered views, cuts or slices of anatomical structures. These underlying tissues are usually obscured when using conventional, plain x-rays, because of the superimposition of more superficial tissues.
In addition, the advantage of a “corrected cut” is the accuracy of the subject anatomy, without artifacts, and its reproducibility before, during and after treatment.
CBCT yields a tremendous amount of even subclinical information about the fossa / condylar relationship and the integrity of the TMJoint mechanism. The Bibliography in this report documents the “refereed literature” of the TMD treating community, recognizing CBCT as the standard of care among the TMD treating community.
At Hawaii TMJ Institute, we use electronic bio-instrumentation to objectively document compromised function (dysfunction)
This part of our essential diagnostic protocol provides the clinician with a wealth of information as to the nature of the dysfunction in the temporomandibular joint. Obviously this information is extremely helpful in determining not only how to treat the dysfunctional joint, but gives the clinician an insight into limitations of treatment.
